Fungal infection is usually attributed to changes in the composition of the oral microbiome due to local and systemic factors that affect the host’s immunity. This promotes the growth, multiplication and entry of fungi into the mucosa that line the oral cavity, leading to opportunistic infection.
Local factors that promote the growth of fungi are dry mouth, mouth breathing, smoking and old infected dentures that are not removed during sleep, while at the level of systemic health, factors that can reduce the immune response include unbalanced diabetes, acquired and inherited immunodeficiencies, hematological disorders, etc. In addition, medications such as antibiotics and corticosteroids can lead to the development of candidiasis.
From the above mentioned it is clear that the patient’s history in combination with a detailed examination of the mouth can lead to the diagnosis of fungal infection. In fact, a cytological smear may be taken to confirm the diagnosis, the examination of which reveals the presence of fungi in increased numbers.
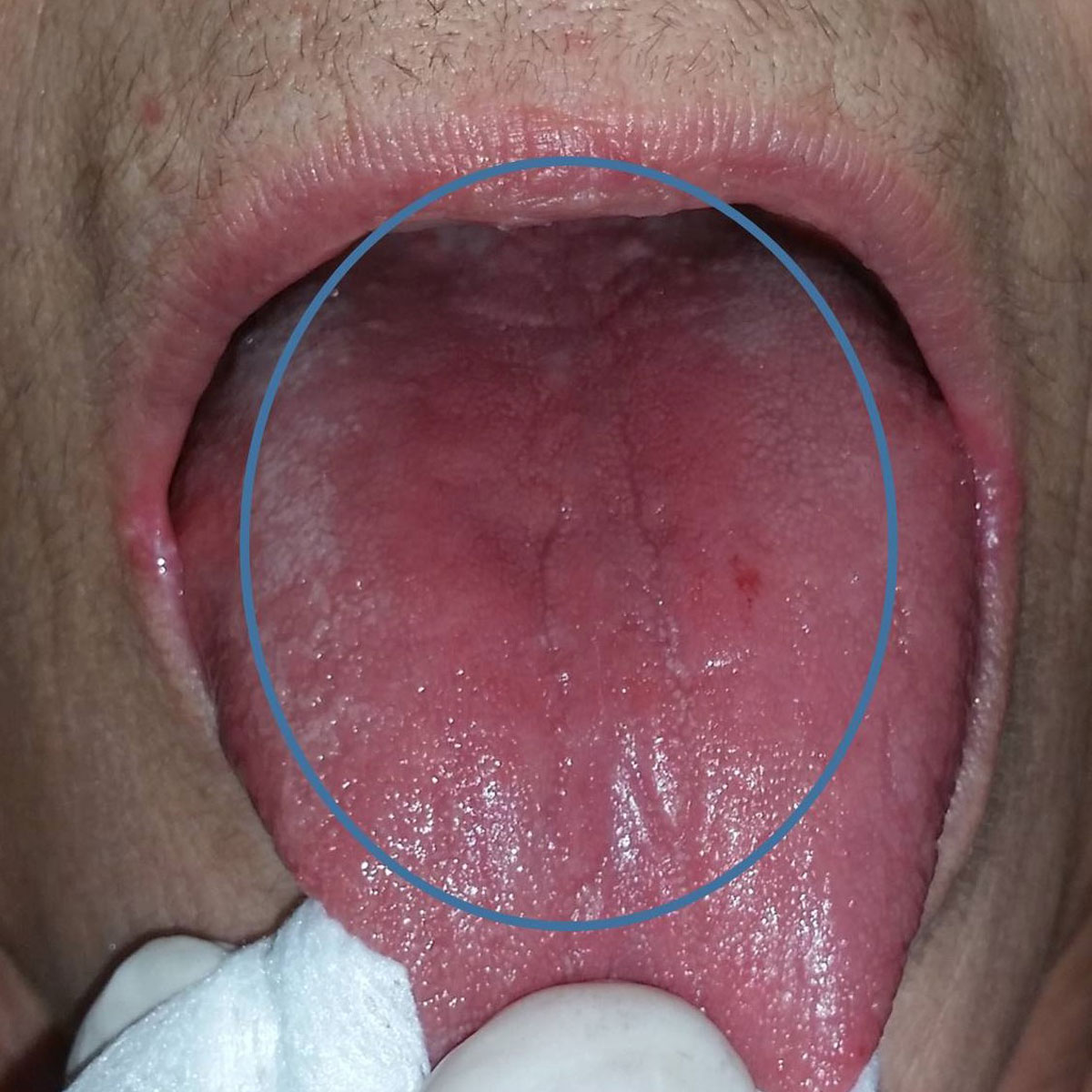
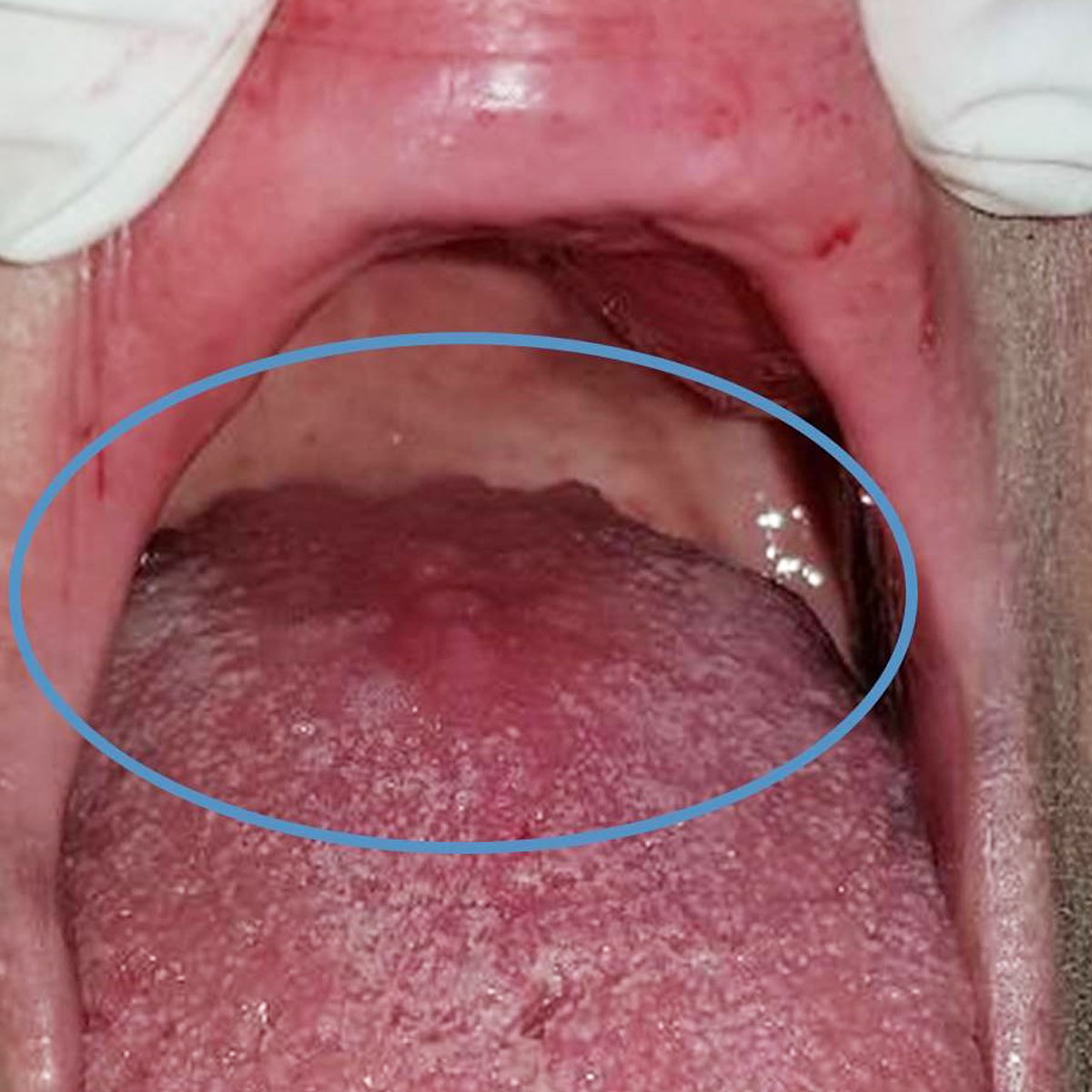
Clinically, redness is observed in the affected areas of the mouth, which usually concern the dorsal surface of the tongue, the palate and the corners of the mouth. In another clinical form of candidiasis, milky white plaques that can be detached are observed. In several cases the patient complains of a mild burning symptom sometimes accompanied by changes in taste such as experiencing bitter, metallic, or saltiness.
Therapeutically speaking, the administration of topical, systemic or in combination with antifungal drugs with a specific dosage and duration of application will lead to the reversal of the damage caused by fungal lesions in the oral cavity. At the same time, the local or systemic cause that is considered to be related to this situation is treated appropriately.